Hidden, Silent Reflux May Be Damaging Your Throat
Dr. Michael Ruscio is a DC, Naturopathic Practitioner, researcher, and clinician. He serves as an Adjunct Professor at the University of Bridgeport and has published numerous papers in scientific journals as well as the book Healthy Gut, Healthy You. He also founded the Ruscio Institute of Functional Health, where he helps patients with a wide range of GI conditions and serves as the Head of Research.How to Tell If You Have Silent Reflux and What to Do About It
- Silent Reflux, Acid Reflux, and GERD|
- Silent Reflux Symptoms|
- Causes|
- How to Address Silent Reflux|
- The Bottom Line|
- Recommended Products|
Download this Episode (right click link and ‘Save As’)
Silent reflux is a condition that often hides in plain sight. If you have a chronic cough, frequent throat clearing, or often have a sore throat, you may have silent reflux.
Reflux means your stomach contents come back up into your throat, which for many people causes heartburn. In silent reflux, heartburn may not happen, leaving you unaware that there is a problem. But this doesn’t mean that your throat and voice aren’t being damaged.
In this article, we’ll define silent reflux and its related conditions, GERD and LPR, describe what can cause silent reflux, and share the research-backed strategies to improve silent reflux and heartburn.

What Are Silent Reflux, LPR, Acid Reflux, and GERD?
Reflux is when contents of the stomach regurgitate into the esophagus or throat. There are several terms used for closely related reflux conditions:
- Silent reflux primarily affects the voice box and the back of the throat or sinuses. It’s called silent reflux when the burning pain associated with acid reflux and heartburn isn’t present.
- LPR (laryngopharyngeal reflux) is simply the medical term for silent reflux. “Laryngo” means something that affects the larynx or voice box, and “pharyngeal” means something that affects the area at the back of the throat, called the pharynx.
- Acid reflux is similar to silent reflux, but the defining symptom is burning pain in the throat or heartburn.
- GERD (gastroesophageal reflux disease) is a more advanced dysfunction of the esophagus caused by prolonged damage to the throat from untreated reflux.
Silent Reflux Symptoms
Silent reflux symptoms primarily affect the voice box (larynx), back of the throat, and sinuses. If you have many of the following symptoms, you may want to be evaluated for silent reflux [1]:
- Hoarseness or vocal cord inflammation
- Chronic cough or frequent bronchitis
- Regurgitation
- Sore throat
- Throat clearing or tickling in the throat
- Difficulty swallowing
- The feeling of a lump in the back of the throat
- Heartburn
- Postnasal drip
- Sleep disturbance
- Shortness of breath
Untreated, silent reflux can lead to the more serious symptoms or conditions of GERD, which include:
- Chronic vocal injury or scarring of the vocal folds
- Barrett’s esophagus (changes in the skin lining your esophagus), which can lead to a rare esophageal cancer [2]
- Narrowing of the airway just below the vocal cords [3]
- Eosinophilic esophagitis [4]
Silent reflux is usually diagnosed by a gastroenterologist or ear, nose, and throat doctor (otolaryngologist). Diagnosis may be based on medical history or an endoscopy (a test to look at your esophagus and stomach). You can’t see reflux on an x-ray.
If you are having difficulty swallowing, feel a sensation of a lump in your throat, or experience frequent vomiting, please get evaluated by your doctor to rule out anything serious.

What Causes Silent Reflux?
The causes of silent reflux are unique for each person, and there’s not a universally agreed-on cause. But similar to other digestive problems, it can relate to changes like:
- Slowing of your gut motility (the movement of food through your gut) [1];
- Low digestive juices, like stomach acid or digestive enzymes;
- Or poorly functioning sphincters (muscles in your digestive tract that open and close to allow food through). This may allow the contents of your stomach to backflow into your esophagus [1].
For example, a lazy lower esophageal sphincter is often a cause of reflux.
And though there aren’t clear causes, you’re more likely to have silent reflux if you also have these conditions:
- Sleep apnea: A systematic review found that 45% of people with sleep apnea also had LPR [1].
- Hiatal hernia: Occurring when the upper part of your stomach bulges through your diaphragm, this is associated with reflux for about 53% of patients [1].
- Low stomach acid: This is often caused by increased age [5], some autoimmune diseases, or long-term PPI use [6].
How to Address Silent Reflux
If you have silent reflux, it’s important to get treatment to prevent long-term damage to your esophagus and throat.
Conventional treatment for silent reflux usually involves proton pump inhibitors (PPIs) like omeprazole (Prilosec), but many reflux patients don’t experience relief on these medications. Even worse, long-term PPI use is associated with an increase in all-cause mortality [1], cardiovascular problems, and GI infections [7].
A natural approach can often improve or resolve silent reflux and has fewer risks. Let’s explore what can help.
A Natural Approach for Silent Reflux
Reflux can respond well to some diet and lifestyle changes. In simple terms, a natural strategy for silent reflux includes the following steps:
- Modify your diet and eating habits to remove reflux triggers.
- Improve your gut microbiome with probiotics. Address gut infections with antimicrobials if necessary.
- Support your stomach acid with betaine HCL if needed.
- Add additional therapies only if the first three don’t provide relief.
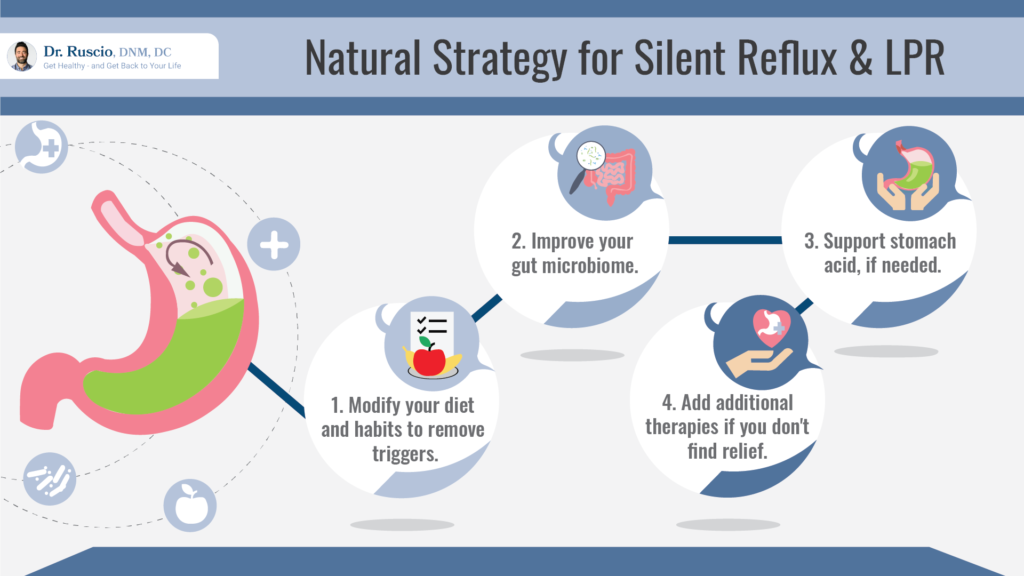
Let’s explore the specifics of this approach.
Diet Advice for Silent Reflux
Certain foods and eating behaviors, like overeating, often aggravate reflux and heartburn.
If you haven’t yet figured out what is making your reflux worse, a simple elimination diet to remove common inflammatory foods is a good place to start. Studies suggest a low-carb diet or a low FODMAP diet may be helpful for GERD, reflux, and heartburn [8, 9, 10]. A low-carb Paleo diet or low FODMAP diet is a great place to start.
Other diet advice that has been shown to be helpful for reflux, GERD, or heartburn is aimed at reducing common symptom triggers. This includes [1]:
- Avoiding oily, acidic, fried, or spicy foods
- Avoiding caffeine and alcohol
- Eating smaller meals to avoid overeating
- Not lying down for several hours after eating [11]
- Elevating the head of your bed several inches by placing blocks under the bed’s top legs.
Ultimately, test any dietary changes for a few weeks. If they don’t make any difference, there’s no need to continue. If they are helping, continue avoiding the foods and behaviors that were triggering your symptoms while you work on other areas.
The Gut Microbiome and Silent Reflux
Some early research suggests that the health of your gut microbiome may be related to reflux. For example, a systematic review found that probiotics appeared to improve several GERD symptoms, including regurgitation, reflux, heartburn, and indigestion [12].
Another systematic review and meta-analysis found that H. pylori, a bacterial infection of the stomach known to cause ulcers, was prevalent in almost half of patients with LPR [1]. This implies that there is an association between H. pylori infection and some LPR cases. On the other hand, H. pylori has been shown to protect against reflux and esophageal cancer in other studies, so the data don’t all agree [1].
In the absence of clear clinical research, we can tentatively infer that improving the gut microbiome with triple probiotic therapy and treating any underlying infections like H. pylori or SIBO may provide reflux relief.

Stomach Acid for Silent Reflux
PPIs like esomeprazole (Nexium), lansoprazole (Prevacid), or H2 blockers (antihistamines like Pepcid AC) are often prescribed for silent reflux to reduce stomach acid.
However, not all evidence agrees that PPIs improve reflux. For example, two systematic reviews and meta-analyses suggest that PPIs improve reflux [13, 14], while a different systematic review found there was no statistical difference for patients between PPIs and a placebo [1].
Ironically, increasing stomach acid improves reflux for some patients. Stomach acid supports many aspects of your digestive function, and a deficiency can contribute to many gut symptoms. Not everyone needs stomach acid, but we’ve seen it make a big difference for some patients at our center for functional medicine. If supplemental stomach acid is right for you, it should lead to noticeable changes in your symptoms. If it doesn’t, supplementation should be discontinued.
You may be more likely to benefit from stomach acid support if you:
- Are over 65 [5]
- Have an autoimmune condition, like Hashimoto’s thyroiditis or rheumatoid arthritis
- Are anemic [15]
- Have been diagnosed with H. pylori
- Have chronically used antacids or proton pump inhibitors (PPIs)
Additional Therapies for Silent Reflux
A few other natural remedies may provide added relief from silent reflux symptoms. Consider bringing these therapies into your routine if diet changes, probiotics, and stomach acid support haven’t made a difference.
- Sodium alginate, a supplement derived from brown kelp, forms a foam raft that acts as a physical barrier between the esophagus and stomach. A systematic review found alginate therapy highly effective for mild GERD [16]. Alginate is the active ingredient in a liquid over-the-counter medication available in the UK called Gaviscon Advance and a relatively new product called Reflux Gourmet.
- Melatonin, a hormone your body produces each night to stimulate sleep, may protect the esophagus for people with GERD and heartburn [17]. Studies suggest melatonin may be as effective as a PPI for improving GERD [18, 19].
- Prokinetic herbs, like Iberogast or RKT (a Japanese herbal blend), improve the movement of food through your digestive tract and may improve reflux, heartburn, and lower esophageal sphincter function [16, 20, 21, 22, 23, 24, 25].
Surgical Treatment for Silent Reflux and Hiatal Hernia
Hiatal hernia — when the upper part of your stomach bulges through a tear in your diaphragm (the muscle at the bottom of your rib cage that drives your breathing) — is associated with reflux in about 53% of cases [1].
One study compared a surgical treatment called fundoplication to PPI therapy alone for patients with LPR and hiatal hernia. Fundoplication was found to be more effective for improving cough, throat clearing, and improved quality of life for patients with LPR [26]. Most patients who were treated surgically were able to discontinue PPI therapy.
In addition, some chiropractors and osteopaths are skilled at adjusting a hiatal hernia, which may give some temporary relief of hiatal hernia-related reflux symptoms.
The Bottom Line
If you have chronic symptoms like a frequent cough, throat clearing, or a sore throat, silent reflux may be the reason for your symptoms.
Instead of taking prescription medications that may have serious side effects, focus on root cause solutions like removing your food triggers, rebalancing your gut microbiome, and supporting stomach acid first. Consider additional therapies if these strategies don’t work to prevent damage to your esophagus.
With some dedicated attention to these details, you can improve silent reflux and protect the long-term health of your voice and throat.
Sponsored Resources
Hi everyone. After many requests, we’re very excited to announce we have two brand new flavors of our best-selling Elemental Heal. Elemental Heal, in case you haven’t heard of it, is our great-tasting, meal replacement, hypoallergenic, gut healing formula. These formulations and flavors aren’t ones you’ll find anywhere else, and better yet you do not need a doctor’s note to order or use them. In addition to our existing varieties, we now offer Peach in the whey-free version and Vanilla and the low-carb version. These have been through some serious tastes tests, so we really think you’re going to enjoy them. Whether you’re using Elemental Heal as a morning shake meal replacement, as a mini gut reset for a few days, or even using it exclusively for two to three weeks, we now have a formula that should fit your needs.
If you go to DrRuscio.com and head to the store, we’re offering 15% OFF any one of our Elemental Heal formulas. This discount is limited to one per customer. Simply use code “TryElementalHeal” at checkout and you’ll get that 15% OFF. Let us know what you think about the new flavors. We believe that you’ll find them to be not only great tasting, but also really friendly on the gut and can help give you a boost in how you’re feeling.
➕ References
- https://www.niddk.nih.gov/health-information/digestive-diseases/barretts-esophagus
- https://www.hopkinsmedicine.org/otolaryngology/specialty_areas/complex_airway/conditions/subglottic_stenosis.html
- Spechler SJ. Gastroesophageal Reflux Disease and Eosinophilic Esophagitis. Gastroenterol Hepatol (N Y). 2019 Feb;15(2):111-113. PMID: 31011306; PMCID: PMC6469260.
- Thomas G. Guilliams, PhD; Lindsey E. Drake, MS. Meal-Time Supplementation with Betaine HCl for Functional
Hypochlorhydria: What is the Evidence? Integrative Medicine. Vol. 19, No. 1. February 2020. - Chubineh S, Birk J. Proton pump inhibitors: the good, the bad, and the unwanted. South Med J. 2012 Nov;105(11):613-8. doi: 10.1097/SMJ.0b013e31826efbea. PMID: 23128806.
- Jessica Devitt, MD Corey Lyon, DO Sarah Beth Swanson, MD Kristen DeSanto, MSLS, MS, RD. What are the risks of long-term PPI use for GERD symptoms in patients > 65 years? MDedge, J Fam Pract. 2019 April. 68(3):E18-E19.
- Austin GL, Thiny MT, Westman EC, Yancy WS Jr, Shaheen NJ. A very low-carbohydrate diet improves gastroesophageal reflux and its symptoms. Dig Dis Sci. 2006 Aug;51(8):1307-12. doi: 10.1007/s10620-005-9027-7. Epub 2006 Jul 27. PMID: 16871438.
- Yancy WS Jr, Provenzale D, Westman EC. Improvement of gastroesophageal reflux disease after initiation of a low-carbohydrate diet: five brief case reports. Altern Ther Health Med. 2001 Nov-Dec;7(6):120, 116-9. PMID: 11712463.
- Piche T, des Varannes SB, Sacher-Huvelin S, Holst JJ, Cuber JC, Galmiche JP. Colonic fermentation influences lower esophageal sphincter function in gastroesophageal reflux disease. Gastroenterology. 2003 Apr;124(4):894-902. doi: 10.1053/gast.2003.50159. PMID: 12671885.
- Newberry C, Lynch K. The role of diet in the development and management of gastroesophageal reflux disease: why we feel the burn. J Thorac Dis. 2019 Aug;11(Suppl 12):S1594-S1601. doi: 10.21037/jtd.2019.06.42. PMID: 31489226; PMCID: PMC6702398.
- Cheng J, Ouwehand AC. Gastroesophageal Reflux Disease and Probiotics: A Systematic Review. Nutrients. 2020 Jan 2;12(1):132. doi: 10.3390/nu12010132. PMID: 31906573; PMCID: PMC7019778.
- Lechien, J.R., Saussez, S., Schindler, A., Karkos, P.D., Hamdan, A.L., Harmegnies, B., De Marrez, L.G., Finck, C., Journe, F., Paesmans, M. and Vaezi, M.F. (2019), Clinical outcomes of laryngopharyngeal reflux treatment: A systematic review and meta‐analysis. The Laryngoscope, 129: 1174-1187. https://doi.org/10.1002/lary.27591
- Wei C. A meta-analysis for the role of proton pump inhibitor therapy in patients with laryngopharyngeal reflux. Eur Arch Otorhinolaryngol. 2016 Nov;273(11):3795-3801. doi: 10.1007/s00405-016-4142-y. Epub 2016 Jun 16. PMID: 27312992.
- Andrea L Betesh, Carol A Santa Ana, Jason A Cole, John S Fordtran, Is achlorhydria a cause of iron deficiency anemia?, The American Journal of Clinical Nutrition, Volume 102, Issue 1, July 2015, Pages 9–19, https://doi.org/10.3945/ajcn.114.097394
- Huestis MJ, Keefe KR, Kahn CI, Tracy LF, Levi JR. Alternatives to Acid Suppression Treatment for Laryngopharyngeal Reflux. Ann Otol Rhinol Laryngol. 2020 Oct;129(10):1030-1039. doi: 10.1177/0003489420922870. Epub 2020 May 25. PMID: 32449369.
- Bang CS, Yang YJ, Baik GH. Melatonin for the treatment of gastroesophageal reflux disease; protocol for a systematic review and meta-analysis. Medicine (Baltimore). 2019 Jan;98(4):e14241. doi: 10.1097/MD.0000000000014241. PMID: 30681611; PMCID: PMC6358381.
- Kandil TS, Mousa AA, El-Gendy AA, Abbas AM. The potential therapeutic effect of melatonin in Gastro-Esophageal Reflux Disease. BMC Gastroenterol. 2010 Jan 18;10:7. doi: 10.1186/1471-230X-10-7. PMID: 20082715; PMCID: PMC2821302.
- Pereira Rde S. Regression of gastroesophageal reflux disease symptoms using dietary supplementation with melatonin, vitamins and aminoacids: comparison with omeprazole. J Pineal Res. 2006 Oct;41(3):195-200. doi: 10.1111/j.1600-079X.2006.00359.x. PMID: 16948779.
- Rösch W, Vinson B, Sassin I. A randomised clinical trial comparing the efficacy of a herbal preparation STW 5 with the prokinetic drug cisapride in patients with dysmotility type of functional dyspepsia. Z Gastroenterol. 2002 Jun;40(6):401-8. doi: 10.1055/s-2002-32130. PMID: 12055663.
- Madisch A, Melderis H, Mayr G, Sassin I, Hotz J. Ein Phytotherapeutikum und seine modifizierte Rezeptur bei funktioneller Dyspepsie. Ergebnisse einer doppelblinden plazebokontrollierten Vergleichsstudie [A plant extract and its modified preparation in functional dyspepsia. Results of a double-blind placebo controlled comparative study]. Z Gastroenterol. 2001 Jul;39(7):511-7. German. doi: 10.1055/s-2001-16142. PMID: 11505331.
- von Arnim U, Peitz U, Vinson B, Gundermann KJ, Malfertheiner P. STW 5, a phytopharmacon for patients with functional dyspepsia: results of a multicenter, placebo-controlled double-blind study. Am J Gastroenterol. 2007 Jun;102(6):1268-75. doi: 10.1111/j.1572-0241.2006.01183.x. PMID: 17531013.
- Melzer J, Iten F, Reichling J, Saller R. Iberis amara L. and Iberogast–results of a systematic review concerning functional dyspepsia. J Herb Pharmacother. 2004;4(4):51-9. PMID: 15927925.
- Saller R, Pfister-Hotz G, Iten F, Melzer J, Reichling J: Iberogast(r): Eine moderne phytotherapeutische Arzneimittelkombination zur Behandlung funktioneller Erkrankungen des Magen-Darm-Trakts (Dyspepsie, Colon irritabile) – von der Pflanzenheilkunde zur «Evidence Based Phytotherapy».Eine systematische Übersicht. 2002;9(suppl 1):1-20. doi: 10.1159/000068645
- Melzer J, Rösch W, Reichling J, Brignoli R, Saller R. Meta-analysis: phytotherapy of functional dyspepsia with the herbal drug preparation STW 5 (Iberogast). Aliment Pharmacol Ther. 2004 Dec;20(11-12):1279-87. doi: 10.1111/j.1365-2036.2004.02275.x. PMID: 15606389.
- Zhang C, Hu ZW, Yan C, Wu Q, Wu JM, Du X, Liu DG, Luo T, Li F, Wang ZG. Nissen fundoplication vs proton pump inhibitors for laryngopharyngeal reflux based on pH-monitoring and symptom-scale. World J Gastroenterol. 2017 May 21;23(19):3546-3555. doi: 10.3748/wjg.v23.i19.3546. PMID: 28596691; PMCID: PMC5442091.








Discussion
I care about answering your questions and sharing my knowledge with you. Leave a comment or connect with me on social media asking any health question you may have and I just might incorporate it into our next listener questions podcast episode just for you!